Consistent Training Leads to Skilled Running Most athletes will attest that consistency is the most important aspect in progressing fitness and skill through training. This is why injuries set you back from reaching your full potential, or at least reaching goals in a timely fashion. While running, there are many things we can do to prevent injuries and some of them require very little time to implement, although learning the most effective way to implement them is individualized and may take years to achieve personal efficiency. Indeed, running is a skill, and it takes a long time to learn how to use your body in the most effective way. With a good training plan you will improve your efficiency, which will reduce physical and mental fatigue, reduce injury risk, and ultimately improve your performance! If you are new to running, or are simply wanting to improve, try these movement tweaks the next time you head out the door. N.B . These tweaks are good guidelines, but if you have a preexisting dysfunction (remember a dysfunction may not present with pain or any other symptom), you may benefit from a personalized approach. If you fall into this group, book in for a running assessment or seek guidance from a running coach, or rehab professional with post-graduate training in running assessments. It's Much More Than One Foot in Front of The Other 1) Upright posture. "Be tall!" At the start of your run, and periodically during your run, remind yourself to be tall. Think about elongating your entire spinal column; That is... if you had a string attached to the top of your head that connects down through the middle of your body, think about pulling that string up! You should not dramatically change your spinal curve with this, but you should feel that you are slightly taller. Why? When done appropriately, this helps to engage your multifidus muscles (spinal stabilizers), and make you aware of your core. This will help prevent energy loss due to poor stability, and will better allow you to apply force through your hips - helping to propel you forwards. It also helps with diaphragmatic activation and reduces the amount of airway resistance during breathing. PS - it might be a good idea to start thinking about upright posture during the rest of your day, as we spend thousands of hours hunched over at work and at home each year, and BELIEVE IT OR NOT!, this affects our athletic performance! 2) Forward lean from the feet / ankles "Lean forward from the ankles!" Running should be efficient. Leaning forward from the ankles aids in this efficiency, because it moves your center of mass slightly forward, and allows you to fall into your next stride. Don't forget #1 - it is too easy to let your forward lean come from hinging at the hips - "Stay Tall", and keep your head up, as you need to be looking forward! 3) Posterior-chain propulsion "Push, don't pull!" If we lean forward from the ankles, we will fall forward and must flex our hip joint and extend our knee to "catch" us from falling on our face. We can use this forward energy most effectively by pushing ourselves forward, as soon as our foot hits the ground. Try to see if you can feel yourself pushing forward using your glutes, hamstrings and calves. 4) Shortened stride and increased cadence "Shorten your stride and increase your cadence!" "Imagine that you are a ball, and as you are rolling over the ground, you are attempting to touch as many different places on the ground as possible" Most research suggests that elite runners who stay injury-free run with a cadence between 160-190 BPM. In most runners this improves multiple metrics (decreased "breaking phase", decreased vertical oscillation, decreased need for force absorption), and ultimately it decreases the amount of wear and tear / abuse placed on joints and muscles. In addition, it is said to improve efficiency in the long-term after the athlete adjusts to running in this way. The best place for our foot to land is directly under our center of mass because it minimizes the "breaking phase". The breaking phase is best described as wasted energy in the time between the foot striking the ground, and the push off phase when we propel ourself forwards. To ensure that we land with a vertical tibia - it is crucial to having a high cadence and a shortened stride. 5) Land with your foot under your center of mass "Most often, you should land using a midfoot strike" The jury is still out on what the best type of foot strike looks like in endurance athletes, but here is what we do know: A) A midfoot strike is mostly likely to place the foot under your center of mass while running on flat ground. B) Landing with a forefoot strike lends to a 2.6 times decrease in injury risk compared to rearfoot strikers (1). C) Landing on the forefoot or midfoot places more stress on the foot musculature and Achilles tendon. Landing on the rearfoot places more compressive loading forces at the tibiofemoral and patellofemoral joints of the knee. C) Rearfoot strikers tend to land with their foot in front of the body, which leads to have a longer stride and greater vertical loading (increased forces applied to the body) (2). D) Wearing shoes with larger heels lends to heel striking, whereas taking shoes off leads to landing on the forefoot or midfoot, with the strike being closer to the body. As always, we are reminded that science has limitations and common sense prevails, therefore do what feels right... BUT my recommendation would be to run on variable terrain, AND: A) As you run uphill, strike with your forefoot or midfoot. B) As you run the flats, strike mostly with your midfoot. C) As you run downhill, midfoot or heel strike may be best. Concluding Remarks These are but a few ways to immediately change your running form, in an effort to improve efficiency and promote injury-free training. General recommendations are terrible because they assume that all people are alike, so make no mistake - it is probably best to have a running assessment done to determine whether you truly need to change your running form. Nevertheless, exposing yourself to learn different styles of running will grow your running skill-sets and your body's durability, ultimately making you a better athlete! References 1) Daoud, Adam I., et al. "Foot strike and injury rates in endurance runners: a retrospective study." Med Sci Sports Exerc 44.7 (2012): 1325-34.
2) Williams III, Dorsey S., Irene S. McClay, and Kurt T. Manal. "Lower extremity mechanics in runners with a converted forefoot strike pattern." Journal of Applied Biomechanics 16.2 (2000): 210-218.
0 Comments
I've had several clients ask what the initials stand for after my name. This is a great question as it can be difficult for clients, and clinicians across Canada and the rest of the world to stay informed on the latest and/or greatest in qualifications and designations. Although more initials following a physiotherapists' name may mean that they have completed more training, some qualifications require more intensive training, may be more widely accepted as an industry standard, or may be more relevant to patient needs. This article should serve to provide you with a basic level of knowledge, and will give you additional resources if you wish to do further reading! This article will not, however, provide you with a background on all available credentials, as there are dozens of courses that provide continuing education and do not have acronyms that can be used after a clinicians name. Rules & Regulations enforced by College of Physiotherapists 1) Only Registered Physiotherapists are allowed to use the initials of PT or RPT. In the most simple signature, a physiotherapist may use these initials after their name (E.g. Jacob Carter, PT). 2) Typically the first 1-3 sets of letters seen after a Physiotherapist's name will be their university qualifications. BPT (Bachelor of Physiotherapy) BScPT (Bachelor of Science in Physiotherapy) MPT (Master of Physiotherapy) MScPT (Master of Science in Physiotherapy) DPT (Doctor of Physiotherapy) tDPT (Transitional Doctor of Physiotherapy) All physiotherapists will hold a Bachelor Degree. Prior to 2012, Physiotherapists were only required to obtain a Bachelor Degree of Physiotherapy. As of 2012, the minimum required competency to enter the profession is now a Masters degree. For example, I was required to complete a four year Bachelors degree in a health science field prior to two full years of intensive studying during my Masters degree. The previous system did not require the more liberal/background education - instead the four year Bachelor of Physiotherapy degree focused on a specific and applicable curriculum. As of 2020, the United States requires all physiotherapists to hold a Doctor of Physical Therapy. This is pushing the industry standards higher, and I believe that you will gradually see more Physiotherapists in Canada that hold this level of education. Perhaps one day, you will see that Physiotherapists in Canada are required to hold this level of education as well. Additional Information: Physiotherapy Alberta College of Physiotherapists of Ontario Manual Therapy Designations 1) FCAMT (Federation of Canadian Academy of Manipulative Therapists) / FCAMPT (Federation of Canadian Academy of Manipulative Physiotherapists) This has been an industry standard for the last few decades. To become certified is a rigorous process as it is internationally standardized and tested by world leaders in Physiotherapy. The program teaches extensive theory and application techniques as related to functional anatomy, human movement, and manual therapy. Its most common criticism is that there is too much of an emphasis on theory, the theory taught is outdated, and excessive classroom time is spent re-teaching previously learned concepts. While I partially agree with this criticism, I would rather too much theory than too little when it comes to safely performing potentially dangerous techniques such as spinal manipulation. Physiotherapists can obtain this credential via two avenues: Option one takes 5 or more years to complete and requires taking seven courses (approx 64 days in classroom with 7 exams), passing an intermediate practical exam, passing a final practical and written exam, and accumulating 150 hours hours of mentorship and peer study. Option two is outlined next (Master of Clinical Science). Additional Information: Canadian Academy of Manipulative Physiotherapy Orthopaedic Division of The Canadian Physiotherapy Association Orthopaedic Division Education 2) MClSc (Master of Clinical Science) Although there are many universities in the world that offer this degree, Canadian Physiotherapists most likely to have taken the part-time, 12 month program taught at Western University in London, Ontario. The program is comprised of course work and clinical mentorship that focuses on neuromuscular dysfunction in which graduates learn spinal manipulation and participate in a research project. Graduates are eligible to apply for the FCAMPT credentials. Additional Information: University of Western Ontario MClSc Program 3) CMT (Certification in Spinal Manipulation), Cert. MT (Advanced Certification in Manual Therapy), Dip. MT (Advanced Diploma in Manual Therapy), DMPT (Doctor of Manual Physical Therapy). The Swodeam Institute was created by Jim Meadows, who has been called one of the top manual therapists in the world. The Swodeam Institute has been offering courses in one form or another since 1985 (including teaching and examining for FCAMPT), but in the last decade has taken his courses to the mainstream audience in Canada and USA. He offers a series of courses that build on knowledge learned in university, and in his course series. To achieve the Dip. MT, students spend 24 days in the classroom but spend extensive time participating in self-directed learning via online and distributed material. The course vision is that self-motivated students will be able to learn as much (or more) compared to the FCAMT certification process, but in less time. Additional Information: Swodeam Institute 4) COMT (Certificate in Orthopaedic Manual Therapy) A 4 week intensive certification offered by 'Manual Concepts' in Perth, Australia that covers spinal and peripheral manipulation (amongst many other techniques). The course offers students learning opportunities from numerous world leading expert clinicians, researchers and teachers. The competition of this course may lead to an accelerated completion of the Masters in Clinical Science (Manipulative Therapy stream) at Curtin University of Technology. Additional Information Manual Concepts Needling Designations 1) GunnIMS (Gunn Intramuscular Stimulation) or CGIMS (Certified Gunn Intramuscular Stimulation) IMS was conceptualized, researched and popularized by Dr. Chan Gunn out of the University of British Columbia in Vancouver, BC. The technique treats neuromuscular pain, and focuses on treating pain centrally (from the source of the nerve at the spinal column) and peripherally (at the source of pain). Physiotherapists that have been practicing for 4+ years, and have completed a certain level of post-graduate training can register with the iSTOP Institute to study GunnIMS. The course consists of 7 days classroom instruction and practice, written and practical exams, and independent study. Additional Information: Gunn IMS 2) FDN (Functional Dry Needling) Kinetacore was founded in 2007 by Edo Zylstra, a clinician, researcher and instructor. Edo based his course development on his previous GunnIMS training at iSTOP, and numerous other philosophies of Trigger Points and Dry Needling. The technique treats neuromuscular pain with the purpose of improving function immediately after treatment. Treatment is similar to GunnIMS and focuses on treating pain centrally (from the source of the nerve at the spinal column) and peripherally (at the source of pain). To obtain this credential you must take Level 1 and Level 2. Physiotherapists that have been practicing for one year can enrol in Level 1. Enrolling in Level 2 requires a full year of applying Level 1 techniques and records of 200 treatment sessions. Both Level 1 & 2 requires two days of classroom instruction and practice, a written exam, practical exam, and independent study. Additional Information: Kinetacore 3) CAFCI (Certified by Acupuncture Foundation of Canada Institute) Acupuncture is an ancient, safe alternative form of medicine. From a western-medical perspective, the needles stimulate the release of endorphins (the body’s natural pain-relieving neurohormones) by inserting needles into specific anatomical points to encourage natural healing. The Acupuncture Foundation of Canada Institute offers acupuncture training & certification to medical practitioners. The completion of their required four courses (including onsite and online components) and exams awards the therapist the letters CAFCI. This course amounts to 200 hours of training, and can be completed in as little time as one year, or at the therapist's desired pace. Additional Information: Acupuncture Canada 4) TCM (Traditional Chinese Medicine) There are many different programs available across Canada to receive this designation. There are some physiotherapists that have obtained this credential. If a Physiotherapist wishes to practice TCM, they often need to book the patient in for a different appointment, as many TCM practices are not recognized by the Physiotherapy College. Traditional Chinese Medicine is not regulated nationwide in Canada, however there are currently five provinces with a mandate to protect the public’s right to safe, competent and ethical services offered by registered TCM Practitioners, TCM Acupuncturists, and/or TCM Herbalists who are members of the regulatory bodies. TCM graduates require 3-5 years of study, and variable amounts of mentorship/study within Canada and Internationally. To be eligible to write the TCM final exams in Canada, students require 3,250 hours of course work and supervised practice/mentorship. Other variations of qualifications include: Registered Acupuncturist (R.Ac.) – 3 year program Registered Traditional Chinese Medicine Practitioner (R.TCM.P) – combined acupuncture and herbology with restrictions - 4 year program Doctor of TCM (Dr.TCM) – combined acupuncture and herbology without restrictions – 5 year program Additional Information: The Chinese Medicine and Acupuncture Association of Canada Soft Tissue Designations 1) ART (Active Release Technique) Dr. Michael Leahy (Chiropractor) started teaching ART over 30 years ago. The premise of the technique is simple - shorten the tissue, apply directional tension with your hand or elbow, and lengthen the tissue or make it slide relative to the adjacent tissue. I believe this is a valuable technique that has been marketed well. In my opinion, ART teaches techniques that can be learned via other means, and for cheaper prices. Clinicians may use the ART credential after their name if they take an ART course every 12 months. Clinicans also have the option to become Full Body Certified, which requires taking three courses: Upper Extremity, Lower Extremity, and Spine. Courses are not offered in Canada very often, and cost a great deal of money! Additional Information: Active Release Technique 2) GT (Graston Technique) Graston is a form of instrument assisted soft tissue mobilization (IASTM) that serves to address fascial restrictions and scar tissue. The system teaches specific techniques and sells instruments to perform the techniques. It is likely the most well known (or well marketed) system of IASTM in the world, as they were pioneers in the technique. In my opinion, Graston teaches many techniques that can be learned via other means, and for cheaper prices. Since IASTM is not a controlled act, any physiotherapy can perform it and call it IASTM instead of Graston. Clinicians may use the initials "GT" after their name after taking the Level 2 course (also known as M2). To do so, they must have completed Level 1 (also known as M1) of Graston, and have purchased Graston tools. Level 1 takes 12 hours of training. Level 2 requires clinicians to attend an additional 14 hour course. Additional Information: Graston Technique Functional Movement Designations 1) FMS (Functional Movement Screen) The FMS was developed by Gray Cook as a screening tool for fitness trainers to use in identifying limitations and asymmetries in clients without pain or known musculoskeletal dysfunction. The test is designed to have clients move in certain ways where weaknesses and imbalances become noticeable if appropriate mobility and motor control is not utilized. Any fitness or healthcare professional can become FMS certified. The Level 1 certification process requires an online course or an onsite course. To use the credential after your name, you must complete Level 2, which requires attending an onsite course. Level 2 covers additional information on the screen learned in Level 1, and focuses on improving movement patterns using corrective exercises. Most onsite courses are offered in the USA - it seems that they instruct in Canada only 1-2 times a year. Additional Information: Functional Movement Screen 2) SFMA (Selective Functional Movement Assessment) The SFMA was also developed by Gray Cook. The SFMA is meant as a tool for medical/rehab professionals to diagnose movement dysfunction, and efficiently discern the root cause for symptoms. The SFMA is meant to be used for clients who have pain with movement, or who have musculoskeletal dysfunction. The approach teaches that dysfunction is either a joint stability, tissue extensibility or motor control problem. The systematic process uses concepts of altered motor control, the neurodevelopmental perspective, and regional interdependence to direct assessment and treatment. A physiotherapist who lists this credential after their name must complete an online seminar, and a 2 day onsite course (with exams). To improve levels of understanding, clinicians can take Level 2 and Level 3. Most onsite courses are offered in the USA - it seems that they instruct in Canada only 1-2 times a year. Additional Information: Selective Functional Movement Assessment Specialty Certifications 1) CHT (Certified Hand Therapist)
Certified Hand Therapists are known for their skill in diagnosing and treating upper extremity (shoulder to hand) dysfunction. They are credentialed through the Hand Therapy Certification Commission (HTCC). Clinicians may use the CHT credential after their name if they pass the Hand Therapy Certification Examination (four hour examination consisting of 200 multiple choice). As of May 2017, Physiotherapists and Occupational Therapists will be eligible to apply for the examination if they have been registered for three years (previously, five years was the minimum). In addition, candidates must have 4000 hours of "hands on" (haha) practice. Additional Information: Hand Therapy Certification Commission 2) Certified Pelvic Health Physiotherapist There are many organizations that teach Pelvic Health / Women's Health / Men's Health courses in Canada and the USA. These courses focus on theory and internal manual therapy techniques. There are varying regulations across Canada, depending on the province. For example, in Ontario you must be approved by the College of Physiotherapists and placed on the specialized roster to provide "internal assessment or internal rehabilitation of pelvic musculature". However, in Alberta, this is not the case. Furthermore, in Alberta there does not appear to be any regulation in place on what courses a physiotherapist must complete to call themselves a Certified Pelvic Health Physiotherapist in Alberta. There are many clinicians that will use this title who have taken a singular course, and conversely, there are many clinicans that may use this title if they have taken multiple courses - Therefore... buyer beware (or at least do your homework!). Additional Information: One of the best well known instructional institutions in Canada is Pelvic Health Solutions College of Physiotherapist of Ontario Physiotherapy Alberta - Note that Pelvic Rehabilitation is not listed as a restricted activity Falling Short of a Full Recovery: Part 2There is a growing body of evidence that demonstrates the effectiveness of physiotherapy. The profession has seen growth that can be largely attributed to ongoing research, higher level of training, expansion of restricted activities (e.g. use of acupuncture needles, performing spinal manipulation, prescribing diagnostic imaging, endotracheal suctioning, etc.), inter-professional collaboration, and the many leaders that advocate for the profession and push it to higher levels. Despite this, in day-to-day practice, we hear from patients that their pain has not improved or that physiotherapy does not work. Why? Let's start by noting that poor adherence is not exclusive to Physiotherapy; It has been identified in many healthcare disciplines, including physiotherapy (Jack, McLean, Moffett & Gardiner, 2010, Martin et al., 2015). Ultimately adherence to treatment has implications on effectiveness, patient wellbeing, and the overall cost of treating the dysfunction in the long term (e.g. costs may bleed into primary healthcare and/or the treatment of other co-morbid conditions). Although there is no accurate data on the number of patients that fail physiotherapy in Canada, individual clinicians and clinics in which I have worked have seen non-adherence rates in the range of 5 to 25%. The validated research that does exist is outdated, is not exclusive to training in Canada, and does not subdivide adherence based on education/credentials, skill-sets employed in treatment, years of experience, etc. Studies indicate widely different non-adherence rates in physiotherapy; Two older studies found that between 14% (Vasey, 1990) and 70% (Sluijs, Kok, Van Der Zee., 1993) of physiotherapy patients did not adhere to the recommended treatment or number of follow-up appointments. The best quality research available on this topic was published in 2010. The authors completed a literature review of 20 studies (that varied in patient demographics, practitioner demographics, assessment of dysfunction, treatment of dysfunction, and every other variable you can think of...) and found that the majority of available research has focused on factors that were in the patient's control. They concluded that "There was strong evidence that poor treatment adherence was associated with low levels of physical activity at baseline or in previous weeks, low in-treatment adherence with exercise, low self-efficacy, depression, anxiety, helplessness, poor social support/activity, greater perceived number of barriers to exercise and increased pain levels during exercise" (Jack, McLean, Moffett & Gardiner, 2010). It is clear that more research is needed on barriers introduced by health professionals and health organizations. Barriers to Success
Clinician understands patient goals: Ask the patient about the circumstances surrounding their injury: Do they need to return to full health for a specific competition or a specific date? Is the patient training for a specific task? What is their required level of function in sport or daily function? Has the patient created a SMART goal? (SMART stands for Specific, Measurable, Attainable, Realistic and Timely). Patient readiness to change: The very motivated patients will likely stand out, but some patients are a bit harder to read. As a result we need to discern their level of motivation, as this directly correlates to their level of commitment in receiving treatment, and to their home exercise program. (E.g. Did they come to physiotherapy because they were told they should by their parents, spouse, coach?) Adequate timeline for rehabilitation: Does the patient have enough time to adequately treat their dysfunction (e.g. A sports competition in 2 weeks may impair the ability for full recovery). Correct pathoanatomical diagnosis of dysfunction: Clinicians should arrive at a precise and accurate diagnosis. Correct diagnosis of related impairments: If the patient has a complex history, the clinician may need to revisit previous injuries to determine stage of healing and any impairments that affect regional interdependence. Treating the dysfunction in the most effective manner: Comprehensive literature reviews indicate that the most effective combination treatment modalities includes exercise, manual therapy (soft tissue release, joint mobilization and manipulation), IMS/dry needling, and pain education. There is evolving evidence that supports shockwave therapy and laser therapy. The evidence found in Western Medical Research is weak (or moderate at best) for the use of ultrasound, TENS, IFC, NMES, and acupuncture. Implications of past medical history, lifestyle choices: Patients may not heal as well or as quickly if they have other co-morbid conditions or impairments, regularly use or abuse drugs/alcohol, do not sleep well, do not eat well, or live in a stressful environment. Alternatively, patients can expect faster resolution if they have a clean bill of health, active lifestyle, healthy diet, sleep well, are proactive, and experience a healthy level of stress in their life. Clinician provides proper education to patient: What is Physiotherapy? What can I expect during the assessment? Why am I having pain? What is 'pain'? Do I have any derangement (actual tissue damage)? What is my prognosis (can I expect a full recovery and how long will it take)? What can I expect during a given treatment? Do I need to do anything at home/in the gym to make a full recovery? How much time do I need to dedicate to this? Clinician motivates patient: Some patients need a little extra help to overcome their injury as they struggle with depression, anxiety, helplessness, poor social supports, or barriers as related to exercise or pain. Getting to know your patients, checking in, and making yourself easy to access (e.g. providing patients with you email address) can make a world of difference. Commitment of time and resources: Some patients can only afford the initial assessment, whereas others happily follow their clinician’s recommendations. It is difficult to discuss finances with a patient, but this information is crucial to developing a proper treatment plan. To indirectly address this variable, I recommend a certain number of treatments based on the assessment findings and the patient's goals. Ultimately this gives control back to the patient, as they are now equipped with the knowledge of their diagnosis and optimal treatment plan. The result is that the patient can make an informed decision on treatment frequency, affordability and their perceived value of the treatment. Lastly, if there are insurance programs that exist and may assist patients in paying for treatment, I will recommend that the patient research potential options. Patient understands clinician: Sometimes medical professionals speak using a lot of medical language (jargon) that is not understood by all patients. Clinicians must allow open communication and have ample time to answer their patients questions. If you are a clinician that runs out of time during an assessment for effective communication, your clients may appreciate if you open additional avenues of communication (E.g. email). Patient is satisfied with lack of pain, but understands they have not fully recovered: If a patient provides me with this explanation, it may be because I have not provided proper education or assessed their function. Alternatively, there may be other variables at play, which means that I need to allocate additional time to chat with the patient and determine underlying reasons. Otherwise, I am happy to accept their informed decision and encourage the patient to follow-up if they have any questions or concerns. Concluding RemarksIn theory, providing an evidence-based, individualized treatment should lead to the best clinical results. In practicality, there are many other variables that clinicians may need to address to treat the patient as a person and achieve real and lasting results. It can be challenging as a clinician to be aware of all of these variables, all of the time. As a result, the clinician and client must create a partnership where open communication absolves barriers and leads to amazing outcomes! ReferencesMartin, L. R., Williams, S. L., Haskard, K. B., & DiMatteo, M. R. (2005). The challenge of patient adherence. Ther Clin Risk Manag, 1(3), 189-199.
Jack, K., McLean, S. M., Moffett, J. K., & Gardiner, E. (2010). Barriers to treatment adherence in physiotherapy outpatient clinics: a systematic review. Manual therapy, 15(3), 220-228. Sluijs, E. M., Kok, G. J., & van der Zee, J. (1993). Correlates of exercise compliance in physical therapy. Physical therapy, 73(11), 771-782. Vasey, L. M. (1990). DNAs and DNCTs—Why do patients fail to begin or to complete a course of physiotherapy treatment?. Physiotherapy, 76(9), 575-578. Patients trust health professionals to accurately diagnose and treat their medical conditions. As a health professional, I aspire to provide the most effective service, which will result in 100% patient satisfaction. Despite the best intentions, some patients fall short of a full recovery. I have written this two part series to share a few clinical pearls with other rehab professionals, and to help lead athletes and members of the public down a path of discovery to expedite recovery. The first article will focus on what I believe to be the constituents of a full recovery. The second article will present common barriers to a full recovery, and how practitioners and patients can overcome them by working together. A Full RecoveryIn theory, a full recovery is simple; my patients must return to their previous level of function. In practice, many different variables must be addressed to ensure success. These variables are first discerned in the initial assessment but are revisited throughout the treatment to ensure a timely recovery. Ultimately when each variable is addressed, this signifies a full recovery (I will address these variables in Part 2). Functional RehabTo ensure that my patients have reached a full recovery, it is mandatory that I look at function during the initial assessment, various midpoints during rehab, and at discharge. It is surprising how often patients remark that only their specific joint was examined without a broader perspective of regional interdependence (how one area of the body affects another). I assess movement on an individualized basis; I change many variables of the tests as related to a patient's injury, acuity, and their goals (e.g. Functional assessment options for a lower body injury screen may include watching the patient stand up from a chair, walk, run, squat, lunge, perform step-ups, perform plyometrics, and/or their specific sport). A great starting point for a clinician may be using a system like the Selective Functional Movement Assessment (SFMA). By the end of treatment the patient should pass all of the criteria for the SFMA, and may graduate onto the Functional Movement Screen (FMS), or other higher level movements specific to their sport. When any limitations in function are found, my next step is to determine why they exist. A true limitation in function will exist for one of three reasons: 1) Joint Dysfunction 2) Connective Tissue Dysfunction or 3) Motor Control Dysfunction (inability to control your body's movement in simple and complex tasks). Moving forward, I will remember patterns of regional interdependence seen during the functional assessment, and use orthopedic (manual therapy) assessment skills to look at joint, muscle, tendon, ligament, fascial, nerve, and vascular function. Psychometric AssessmentLast but not least, I will assess psychometrics (e.g. A patient's readiness to commit to the rehab program, or readiness to return to life, work and sports). This, often forgotten, aspect of rehabilitation is very important; Sometimes after patients 'fall off the horse', it may be difficult to 'get back on the saddle'. To quantify and track progress in psychometrics, objective questionnaires may be used. Alternatively, I may assess this subjectively, during conversation. While I may use both methods depending on the case, my preference is to develop a relationship with my patients where we can have open conversations. I find questionnaires may occasionally delve deeper than my questions, but do not profoundly impact my clinical reasoning or treatment. In addition, the analysis of the results takes time and detracts from time spent conversing with and treating patients. In the case of clients involved in motor vehicle collisions (MVCs) or with the workers compensation board (WCB), these questionairesare often mandatory. Concluding RemarksIn summary, a full recovery encompasses complete return of musculoskeletal health, motor control (e.g. coordination), along with the confidence to use the body in its required environment.
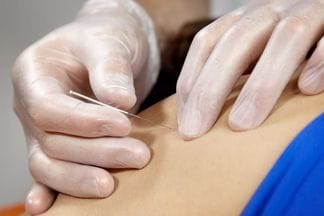
IntroductionThis article is meant to provide education to current clients, future clients, or any other interested parties. It will provide a basic level of knowledge which is available in the current research and should help to answer your question including: "How does it work?", and "Why does my muscle twitch when you put a needle there?!" Intramuscular Stimulation (IMS) is one of the most effective techniques available to reduce muscular pain and tightness; Essentially IMS 'resets' trigger points (TrPs) to allow for normal muscle contraction and relaxation. The technique is known by many names: IMS, GunnIMS, Dry Needling, Functional Dry Needling (FDN), Trigger Point Needling, and Intramuscular Manual Therapy. Regardless of the name, all methods use the same theory and should attain similar results, providing the diagnosis is correct and the practitioner is competent. The most recent systematic review, published in 2015, analyzed 25 high-quality studies and found significant improvement in pain, range of motion, function and quality of life when IMS was used in multiple body regions (1). Its reputation has become well-known: Many advocates from the medical and research community call IMS the most important contribution to pain science and treatment in the last 20 years. As a result it has become a highly sought after skill-set in professional sport, chronic pain centers and physiotherapy clinics everywhere. TrPs have been scientifically acknowledged since the early 1900s, when Sir William Gowers introduced the (now dated) term “fibrositis”, meaning a palpable tenderness and hardness of a muscle. Significant headway was made in the 1970s by Dr. Janet Travell (MD for Presidents Kennedy and Johnson) who authored research documenting TrP pain referral patterns. However, it wasn’t until Dr. Chan Gunn introduced his theories and supporting research in the late 1990s that IMS started to gain formal recognition as a treatment modality. Physiotherapists and physicians with specialized post-graduate training perform IMS. A thorough physical examination proves indispensable as chronic pain is neurologically driven (as opposed to structural), and therefore it is undetectable by X-rays, MRI Tests, Bone and CT Scans. If relevant TrPs are found on examination, a sterile acupuncture needle is then inserted and moved for 1-5 seconds in the tight muscle, causing a cramping or twitch response of the muscle. Needles may also be inserted near the spine where nerve roots have become irritated and hypersensitive. Before we can examine the effects of IMS on TrPs, let's first identify what we know about them. Three Types of Trigger Points There are three types of trigger points: Active Trigger Points – A hyperirritable spot in a taut band of skeletal muscle/fascia which is painful without being touched (but more painful with compression) and produces characteristic pain, referred symptoms, motor dysfunction and/or autonomic nervous system signs/symptoms. Latent Trigger Points – A hyperirritable spot that is painful with compression, but does not have referral symptoms. Satellite Trigger Points – A latent point that develops in a synergist muscle, antagonist muscle, muscle with common neural link or the same pain referral zone. These trigger points may become symptomatic neurogenically or mechanically by an increased irritability of the key TrP. Trigger Point Characteristics Trigger points have been studied thoroughly in the research. Here is what we know to date:
B) Elevated neurotransmitters and neuropeptides involved in pain sensitivity, vasoconstriction, vascular permeability, mast cell degranulation (mast cells release inflammatory components), increased sympathetic activity in motor endplate regions of TrP, decreased feedback control of muscle length and increased spontaneous electrical activity at motor endplates (14). C) Elevated cytokines and chemokines involved in inflammation, immune regulation, sensitivity of nociceptors and increased pain in the muscle (14). Physiological Effects of IMS As we insert an acupuncture needle into a TrP, a reset of the neuromuscular system occurs. This results in reduced local and referred pain (15, 16), improved range of motion (2, 3) and decreased TrP irritability both locally (7, 17) and remotely (8, 18). It is also proposed that these changes reduce associated dysfunction caused by the pulling effects of the tight muscles across joints, discs, nerves, tendons, etc. These results occur for the following reasons:
Conclusion IMS requires a medical examination and diagnosis by a practitioner knowledgeable in musculoskeletal pathology and human anatomy. The technique is supported by high-quality research, and when applied correctly, it can help provide lasting relief to patients with acute and chronic pain. References1) Boyles R, Fowler R, Ramsey D, Burrows E. Effectiveness of trigger point dry needling for multiple body regions: a systematic review. Journal of Manual and Manipulative Therapy. 2015 Jun 18:2042618615Y-0000000014.
2) Lucas KR, Rich PA, Polus BI. Muscle activation patterns in the scapular positioning muscles during loaded scapular plane elevation: the effects of latent myofascial trigger points. Clin Biomechanics. 2010;25(8):765-770. 3) Lucas KR, Polus BI, Rich PS. Latent myofascial trigger points: their effects on muscle activation and movement efficiency. J Bodyw Mov Ther. 2004;8:160-166. 4) Ballyns JJ, Shah JP, Hammond J, Gebreab T, Gerber LH, Sikdar S. Objective sonographic measures for characterizing myofascial trigger points associated with cervical pain. J Ultrasound Med. Oct 2011;30(10):1331-1340. 5) Brückle W, Sückfull M, Fleckenstein W, Weiss C, Müller W. Gewebe-pO2-Messung in der verspannten Rückenmuskulatur (m. erector spinae). Z. Rheumatol. 1990;49:208-216. 6) Ge HY, Fernandez-de-Las-Penas C, Yue SW. Myofascial trigger points: spontaneous electrical activity and its consequences for pain induction and propagation. Chin Med. 2011 Mar 25;6(13):1-7. 7) Kuan TS, Hsieh YL, Chen SM, Chen JT, Yen WC, Hong CZ. The myofascial trigger point region: correlation between the degree of irritability and the prevalence of endplate noise. Am J Phys Med Rehabil. 2007;86(3):183-189. 8) Hsieh YL, Chou LW, Joe YS, Hong CZ. Spinal cord mechanism involving the remote effects of dry needling on the irritability of myofascial trigger spots in rabbit skeletal muscle. Arch Phys Med Rehabil. Jul 2011;92(7): 1098-1105. 9) Rha DW, Shin JC, Kim YK, Jung JH, Kim YU, Lee SC. Detecting local twitch responses of myofascial trigger points in the lower-back muscles using ultrasonography. Archives of physical medicine and rehabilitation. 2011 Oct 31;92(10):1576-80. 10) Chen Q, Bensamoun S, Basford JR, Thompson JM, An KN. Identification and quantification of myofascial taut bands with magnetic resonance elastography. Archives of physical medicine and rehabilitation. 2007 Dec 31;88(12):1658-61. 11) Shah JP, Danoff JV, Desai MJ, et al. Biochemicals associated with pain and inflammation are elevated in sites near to and remote from active myofascial trigger points. Arch Phys Med Rehabil. Jan 2008;89(1):16-23. 12) Shah JP, Gilliams EA. Uncovering the biochemical milieu of myofascial trigger points using in vivo microdialysis: an application of muscle pain concepts to myofascial pain syndrome. J Bodyw Mov Ther. Oct 2008;12(4):371-384. 13) Shah J, Phillips T, Danoff JV, Gerber LH. A novel microanalytical technique for assaying soft tissue demonstrates significant quantitative biomechanical differences in 3 clinically distinct groups: normal, latent and active. Arch Phys Med Rehabil. 2003;84:A4. 14) Shah JP, Phillips TM, Danoff JV, Gerber LH. An in vivo microanalytical technique for measuring the local biochemical milieu of human skeletal muscle. Journal of applied physiology. 2005 Nov 1;99(5):1977-84. 15) Affaitati G, Costantini R, Fabrizio A, Lapenna D, Tafuri E, Giamberardino MA. Effects of treatment of peripheral pain generators in fibromyalgia patients. Eur J Pain. Jan 2011;15(1): 61-69. 16) Srbely JZ, Dickey JP, Lee D, Lowerison M. Dry needle stimulation of myofascial trigger points evokes segmental anti-nociceptive effects. J Rehabil Med. 20110;42(5):463-468. 17) Chen JT, Chung KC, Hou CR, Kuan TS, Chen SM, Hong CZ. Inhibitory effect of dry needling on the spontaneous electrical activity recorded from myofascial trigger spots of rabbit skeletal muscle. Am J Phys Med Rehabil. Oct 2001;80(10):729-735. 18)Tsai C-T, Hsieh L-F, Kuan T-S, Kao M-J, Chou L-W, Hong C-Z. Remote effects of dry needling on the irritability of the myofascial trigger point in the upper trapezius muscle. Am J Phys Med Rehabil. 2010;89(2):133-140. 19) Cagnie B, Barbe T, De Ridder E, Van Oosterwijck J, Cools A, Danneels L. The influence of dry needling of the trapezius muscle on muscle blood flow and oxygenation. Journal of manipulative and physiological therapeutics. 2012 Dec 31;35(9):685-91. 20) Hsieh YL, Yang SA, Yang CC, Chou LW. Dry needling at myofascial trigger spots of rabbit skeletal muscles modulates the biochemicals associated with pain, inflammation, and hypoxia. Evidence-based complementary and alternative medicine. 2012 Dec 23;2012. 21) Niddam DM, Chan RC, Lee SH, Yeh TC, Hsieh JC. Central modulation of pain evoked from myofascial trigger point. The Clinical journal of pain. 2007 Jun 1;23(5):440-8. |
Have you found these article to be informative, helpful, or enjoyable to read? If so, please visit my Facebook page by clicking HERE, or click the Like button below to be alerted of all new articles!
Author
Jacob Carter lives and works in Canmore, Alberta. He combines research evidence with clinical expertise to educate other healthcare professionals, athletes, and the general public on a variety of health topics. Archives
November 2022
Categories
All
|
|
|












 RSS Feed
RSS Feed